About 100 confirmed cases of monkeypox have been discovered from 12 countries across the world. While the incidence of monkeypox cases are nowhere near the number of Covid-19 cases, there are concerns about its spread. What should the public health response be for this disease, which has similarities with smallpox? What is the immunisation strategy that India should follow for this disease?
To discuss this, we spoke with infectious diseases expert Ishwar Gilada, a consultant for HIV and sexually transmitted diseases. He is chairman and managing director, Unison Medicare and Research Centre, Mumbai, and was recently re-elected to the governing council of the International AIDS Society. He is also president of the AIDS Society of India and secretary-general of the People’s Health Organisation-India, a non-governmental organisation that has spearheaded India’s HIV awareness campaign since 1985.
What is monkeypox?
Monkeypox is a virus which is from the same family as smallpox and also vaccinia, which was used for making a smallpox vaccine. Molluscum contagiosum, which we commonly see in sexually transmitted diseases (STD), is also from the same pox variety family. Monkeypox probably originated from smallpox itself, sometime after smallpox was eradicated.
Was smallpox eradicated in India, or all over the world?
Smallpox was eradicated all over the world around 1979-80. Therefore, smallpox vaccination also stopped at that time. There are hardly any manufacturers of smallpox vaccines today, but there are some. I know of at least one of them.
One reason for the fear around monkeypox seems to be that it is also a zoonotic virus, like SARS-CoV-2?
Yes. Monkeypox has originated from animals in the rainforest area of central and west Africa, from squirrels, rats and some monkeys, therefore it is called monkeypox. It was originally located in the west of Africa and Congo, with two different clades. In Cameroon, they have both clades in their monkeypox cases.
Why is monkeypox spreading now? What is triggering the spread?
No one can say with certainty, but monkeypox is definitely out of the endemic zone, which is western and central Africa, and is in non-endemic zones now. Usually, when cases are found in endemic zones, nobody’s concerned because it [circulates] only there, whether in monkeys or in other animals or human beings, and is contained and sustained there itself. But [it’s a concern] when it comes out [of the endemic zone] in large numbers.
READ I Digital health apps: How useful are they?
Currently, it is spreading in individuals without any travel history. As you said, monkeypox was [detected] in 12 countries. Today, it [has been detected] in 19 countries with almost 132 cases diagnosed, and another 100 suspected cases. So it has become a problem as it is out of its endemic zone.
Also, it is spreading faster. As we’ve seen, in the United Kingdom itself there are 56 cases registered. Spain and Portugal have more than 30 cases each. Most cases are in the Schengen country areas, because if you have a Schengen visa, you may land in one country but can travel around 15-16 countries. We are seeing [monkeypox cases] everywhere [in the Schengen area], whether Germany, Italy, Sweden, the Netherlands or Belgium. It started spreading from rave parties in Spain and Belgium. Rave parties are followed by sex parties, thus, sexual transmission was thought of [as the cause] earlier and it is being considered more dangerous than earlier thought.
Monkeypox is transmitted, according to World Health Organization (WHO) descriptions, through close proximity, exposure to bodily fluids and also respiratory droplets, which makes it similar to Covid-19?
Probably the WHO doesn’t want to make the same mistake they did with Covid-19, therefore they’re saying [it spreads through] droplets. At least they didn’t say [it spreads through] aerosols, as it is not possible through aerosols.
READ I Indian economy: War on inflation will warrant sacrifices
A droplet means surface transmission from bushmeat, from rodents, to dogs and cats and from there to domestic animals to human beings. So, [monkeypox is transmitted from] forest animal to domestic animal to human being, and now even human being to human being. [It can spread through] close contact in the family, skin to skin contact, therefore it is also [grouped under] STDs.
Is there a natural body resistance to monkeypox or even a smallpox virus today?
To some extent, yes, because whenever monkeypox is seen in the elderly population, who have been vaccinated for smallpox, symptoms are very few. In the 20- to 40-year-old population, who are not vaccinated against smallpox because vaccination stopped around 1980, the cases are severe. Hence, they realised that smallpox vaccination gives almost 85% protection [against monkeypox], therefore it is thought that smallpox vaccination should be restarted in those areas where it is becoming endemic.
When you say that smallpox vaccination, which could have provided immunity to monkeypox, was stopped in 1979, does that mean that most people born before that time would have been vaccinated, including in India?
Yes, because smallpox was a known disease for 220 years. It was widespread in India and all over the world. Almost 100% were vaccinated. Smallpox was a fatal and disfiguring disease. It left pockmarks for a lifetime. I still see people of my age, or older, with pockmarks.
But when smallpox was eradicated globally, WHO waited for a couple more years, and said not a single case was recorded since 1980. Therefore, smallpox vaccination stopped, but vaccines still exist, for two reasons. One, it was always thought that smallpox can be used in biological warfare, therefore vaccines were needed. There is one company which makes that vaccine. This can also be used for the treatment of rabidpox or monkeypox or other such kinds of pox diseases.
What is the best way to approach monkeypox as a public health challenge? Is it through immunisation, or waiting for cases to turn up and treating them, because it is not potentially as fatal as Covid-19?
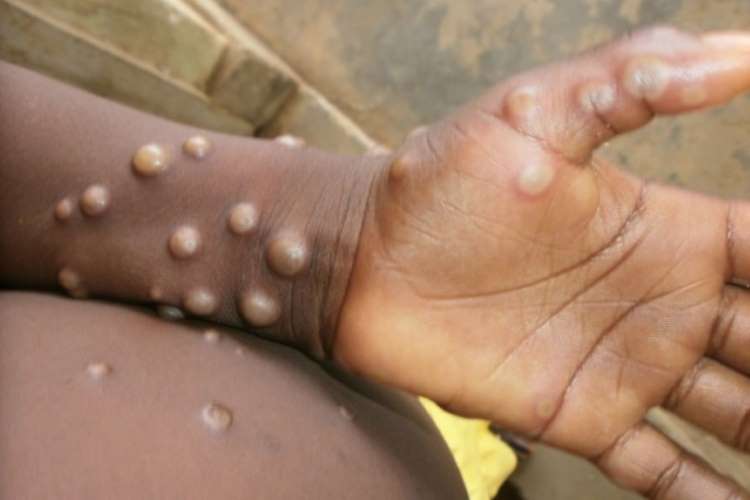
I think ‘wait and watch’ is the best policy. We should also be vigilant. Just using thermal scanners won’t help, because we have not seen any Covid-19 cases detected through thermal scanners. People with fever will just take paracetamol and sit on a flight or a ship. So that is a bygone strategy. We should look for the four or five symptoms of monkeypox, which are present in all cases. One is that people with monkeypox have pockmarks or vesicles or postules on the face, palms and soles.
The palms and soles are affected in 80% to 90% of cases. So at airports, people can be asked to show their palms and soles, and their face in case somebody’s covering their face. Secondly, lymph node enlargement in the neck area is again a symptom in 100% of monkeypox cases. So it will make more sense to be vigilant and check for lymph node enlargement, pockmarks or vesicles, and also persons with fever and travelling from affected areas.
If we do find suspected monkeypox cases, we need to have a differential diagnosis. For instance, at the time of the plague, they started looking for lymph node enlargement in Bombay Central and found some suspected plague cases, but these turned out to be HIV cases. We should check [whether lymph node enlargement] is due to tuberculosis, HIV, Hodgkin’s or non-Hodgkin’s lymphoma, etc. We also have to check whether the pockmarks or vesicles are a reaction to drugs, or due to Herpes zoster, which is seen more commonly in India. So we need to differentiate between monkeypox and these other diseases, but we should be vigilant.
If at all it is monkeypox, currently the smallpox vaccine can be used as a treatment as well. If a person starts developing symptoms, if they get the smallpox vaccine within three to four days, it also works as a therapy. Vaccination can be prophylactic and also therapeutic. We should look at remanufacturing the smallpox vaccine and there’s no better country than India to do that. There are also a couple of antiviral drugs being trialled. Let us see if that will work.
If I wanted a smallpox vaccine today in India, could I get it?
I don’t think you will get it here. There is one company, Bavarian Nordic, which makes the smallpox vaccine. I don’t know whether Indian companies would have it. But if at all they do, there will be expired stock. Some companies may be producing these for some international demand, particularly from Africa. In the US, they found about 70-80 cases of monkeypox around 2003. At that time, there was a demand for these vaccines.
Essentially, India has to scale up and increase smallpox vaccine production if monkeypox were to spread more virulently?
Yes. In the current era, the last 40 years, we are seeing more and more viral infections. Infections are usually of four types: bacterial, fungal, parasitic and viral. We have effective antibacterials, antifungals and anti-parasitics, but there are no effective antivirals, therefore it is a kind of ‘man proposes, God disposes’ scenario. [This is why there are] more and more viral infections emerging and in circulation.
The main thing is that these should not become endemic and a pandemic, as we have seen with Covid-19. That’s the reason why we can’t discount any such outbreak anywhere. From a small place like Wuhan, Covid-19 spread all over the world, and brought the entire world to its knees for at least two years.
We should be vigilant and plan for monkeypox to become a bigger problem, through pandemic preparedness. We should not have a unilateral or microscopic programme addressing only one virus. We should have a pandemic preparedness plan for who should deal with a viral infection which emerges. Rightly so, this time the Government of India roped in the National Centre for Disease Control (NCDC), along with ICMR (Indian Council of Medical Research). For Covid-19, they only roped in ICMR directly. You require a public health approach.
We’ve seen chickenpox in India. Many of us have had chickenpox many years ago. Is there any connection between chickenpox and monkeypox/ smallpox?
Not at all. Chickenpox is a different pox, a different virus. It is a herpes virus, varicella zoster. Herpes zoster is a reactivation of chickenpox and is the same virus. So if you don’t get chickenpox in childhood, you get herpes zoster when older. It is from the same family. Chickenpox is not from the same family as smallpox. Smallpox, vaccinia, molluscum and monkeypox are from the same family.
From a public health perspective, you said India needs to be in pandemic mode, respond swiftly and be alert at all times. What else should we be doing in this new world where zoonotic diseases can arise suddenly, spread fast and reach you faster than you could imagine?
Being a vegetarian myself, I would ask people to be vegetarian. Secondly, if at all you eat meat, you should not eat raw meat. Third, there has to be some limitation [or distance] between [human] habitation and wild animals. If wild animal areas are also inhabited by human beings, then there are likely risks of infections in wild animals getting transmitted to human beings or domestic animals.
We should be vigilant about this. Wherever there are rodents moving around, bush meat, or wild animals in domestic animal areas, there are bound to be problems. There’s no one single answer to this. But we should either not eat meat, and if at all we do, then it should be completely cooked rather than raw.
These viral diseases are also spreading between countries. For instance, monkeypox originated in a more tropical area and other zoonotic diseases may originate in other parts of the world. Travel, thus, is obviously a critical contributor to the spread of any virus?
No, I don’t think there’s any contributory factor other than the globalisation of everything. Anything which is available in one part of the world will go to other parts of the world. There are a lot of theories around ‘cold area-hot area’, ‘tropical area-non tropical area’ etc. They did not hold any good for Covid-19. So, we cannot say that it will work well for another new infection also.
Secondly, the world is wiser than two-and-a-half years back, so [countries] would definitely take some kind of containment measures [around travel] thoughtfully. The Indian government also is responding and a lot of cities, ports and airports are being put on alert so that we can contain [monkeypox cases] as early as possible.
Otherwise, keeping good immunity, keeping your comorbidities under control is very important, because any new infection arising will affect people with comorbidities and not maintaining good immunity more. We should not only maintain good immunity during the time of pandemics, but always.
India had the national smallpox eradication programme in 1962, which focused on outbreaks. Any lessons from that to apply to today?
I don’t think any one lesson can be learned from that time. Things were different at that time and different now because of globalisation. There are more challenges now than earlier. People were docile at that time. You created a containment zone and people would stay within it. In this era, people don’t want to stay in containment zones. A containment zone is [seen as] a kind of stigmatisation.
All the stories I learned from my parents and grandparents about that time were how they were kept separately in a small hut. Houses, areas, cities or towns were sealed. [Authorities] used to mark one cross on [a house where there was] one death, two crosses where there were two deaths. Now, people will not listen. So those eras were different, and this era is different. We need to look at two things: vaccination and treatment. Also, we should develop more and more antivirals, as there are more possibilities now because of some new techniques which have been developed. We should invest in that.
(Published in an arrangement with IndiaSpend.)
Govindraj Ethiraj is a journalist and entrepreneur based in Mumbai. He has over 25 years experience with India's top print and TV platforms. He is the founder of public interest journalism ventures such as IndiaSpend, FactChecker and BOOM.

