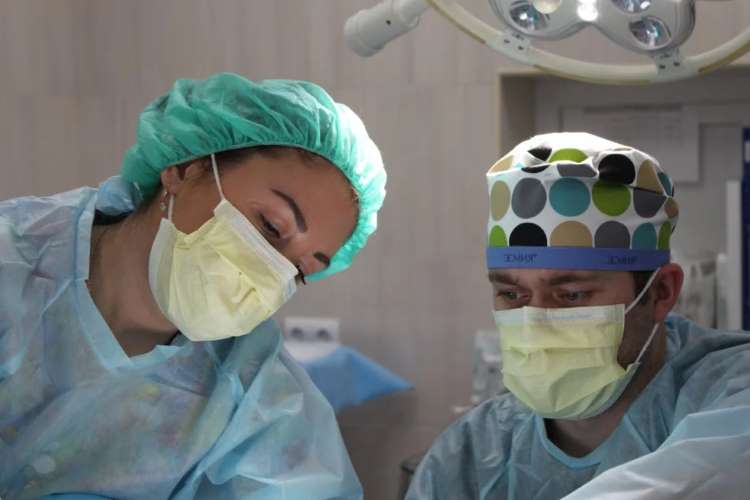
With fears of another outbreak of the covid 19 pandemic looming large, the government has an onerous task of strengthening the country’s public health system. The healthcare sector in India is one of the most neglected areas and the fault lines were exposed by the second wave of covid 19 which resulted in thousands of deaths across the country. Many Indians won’t forget the haunting images of dead bodies floating in rivers. The Union Budget offers an opportunity to the government to make decisive steps towards building a healthcare infrastructure accessible to all citizens.
The Economic Survey 2021 had suggested that the government should spend at least 2.5-3% of the GDP in healthcare. The survey said private health insurance expenditure has jumped from 1.6% (2004-05) to 6.6% (2018-19) over a period of 15 years. While the government expenditure on health has increased considerably, the out-of-pocket expenditure of citizens on health remains high.
India public health expenditure
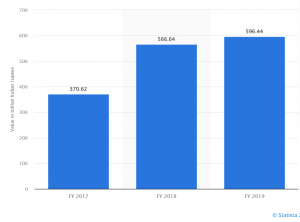
Issues plaguing public health system
The Indian healthcare industry is at least $372 billion in 2022, according to IBEF. The size of the industry has never been a problem, but lack of access renders any progress in the sector irrelevant to most citizens. Many people in India, particularly those living in rural areas, do not have access to quality healthcare due to limited number of hospitals and healthcare facilities. This leads to long waiting times and lack of access to timely treatment.
READ | Gathering storms: Contraction of UK economy stokes deep recession fears
Then there is the issue of shortage of healthcare professionals including doctors, nurses, and other medical staff. According to the latest data available with the World Healthcare Organisation (WHO), the number of physicians available for 1,000 people is less than 1. The Euro area has 5.5 physicians for every 1,000 people. Cuba and Italy have as high as 8 doctors per thousand. Lesser number of healthcare professionals leads to a lack of access to care, as well as an increased workload for those professionals who are available.
The high cost of treatment has also been a major deterrent to availing equitable healthcare. Treatments for various conditions can be expensive, especially for those who do not have access to insurance. This prevents people from seeking the medical care they need. Poor infrastructure in many healthcare facilities is also an issue.
The health budget needs a major overhaul to protect citizens from plunging into poverty due to debt related to unexpected medical expenses. Over 40% of health expenditure is on medicines and pharmaceuticals. Any improvement in this area will be a significant achievement. Preventive healthcare expenditure has remained dismally low despite enough evidence to show that mass preventive screening can bring down overall healthcare costs in the long run.
The Union Budget is just round the corner and the healthcare industry wants the government to give adequate importance to public health to reach the pre-pandemic levels in terms of numbers. The industry also has several suggestions which need urgent follow up. These suggestions include channelling CSR funds to healthcare and giving a fillip to start-ups in the sector.
For one, there are more than 4,000 start-ups registered in the healthcare space, but the larger challenge of affordability and accessibility remains a constant concern. While companies have ample CSR funds, a lack of access to both public and philanthropic funds is worrisome.
Industry insiders say the government must now push for a Unified Health Interface connecting all public and private medical establishments. UHI will facilitate data exchanges between different sources of information such as hospitals, primary care centres, and laboratories. This will help in collating information from disparate sources so that data can be exchanged in real time.
That the government needs to increase budget outlay for the healthcare sector has been a topic of discussion for decades. But it also needs to target spending on public private partnerships and move from a provider role to an enabler role. This will help in delivering quality healthcare to masses in quick time.
The government also needs to address the issue of lack of credibility of medical laboratory professionals and allied health professionals. In absence of any regulatory legal mechanism to oversee the educational and professional standards, educational institutions have been growing at a rapid rate. It is time for a corrective step to handle this issue.
READ | Zero covid policy: China’s folly to haunt global economy
As the head of G20, India is putting a lot of emphasis on health. Health has been a priority area for the grouping since 2017. G20 holds an annual meeting of health ministers. The destruction caused by Covid 19 in terms of lives and livelihoods has infused some sense of urgency to the cause.
Universal Health Coverage, a concept originated in the early 2000s, has been adopted as a pathway towards Sustainable Development Goal 3. The UN General Assembly accepted the UHC-PHC approach in 2019 as a political declaration. The success of public health centres during the pandemic triggered a rethinking among policy makers. As the private medical system is unaffordable to a majority of citizens, the PHC-UHC approach can improve access by linking primary healthcare and preventive action.
India can put forward its national health mission as an example other country can emulate. The country has done well in tackling malaria and HIV infections. India needs to walk the talk in providing public healthcare by improving funds flow to this key sector.

